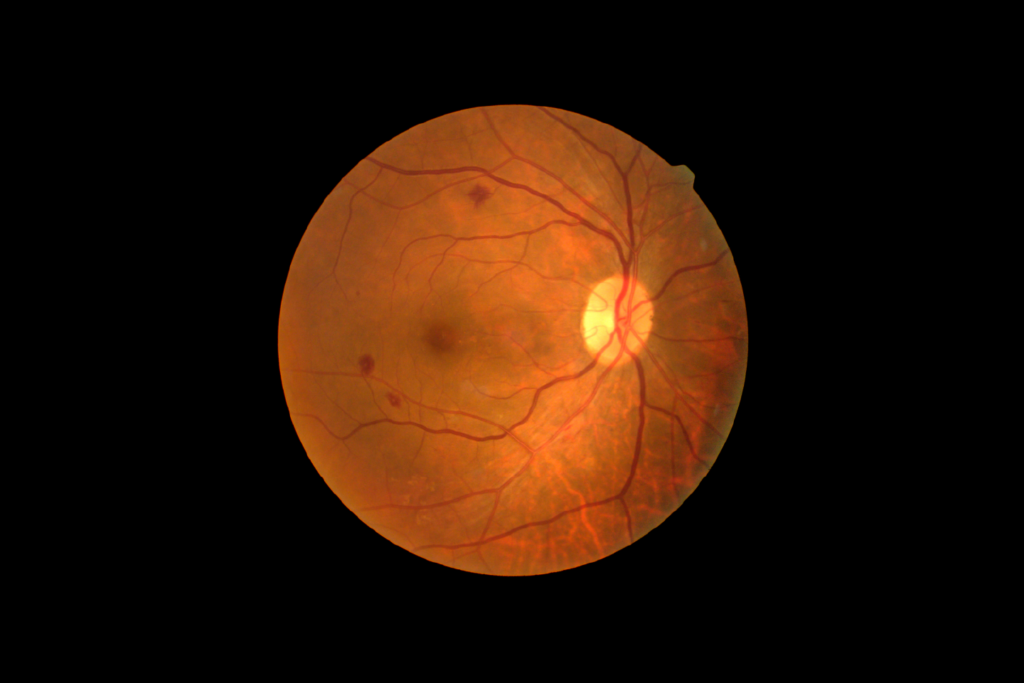
Diabetes affects more than blood sugar levels-it can also have serious consequences for eye health. One of the most significant complications is diabetic retinopathy, a condition that damages the small blood vessels in the retina. The retina is responsible for capturing light and sending visual signals to the brain, making it essential for clear sight.
Because early stages often develop without noticeable symptoms, many people are unaware that their vision is at risk. Recognizing warning signs early can prevent permanent damage and protect long-term eyesight.
The Silent Nature of Early Disease
One of the most concerning aspects of diabetic retinopathy is that it may remain silent for years. You may feel that your vision is normal while subtle damage is occurring beneath the surface. By the time noticeable symptoms develop, the disease may already be in an advanced stage.
That is why annual dilated eye exams are strongly recommended for individuals with diabetes. Early detection significantly improves treatment outcomes.
Why Early Detection Matters
In its initial stages, retinal damage may not cause pain or obvious visual changes. However, as the condition progresses, weakened blood vessels can leak fluid or bleed into the retina. This disrupts the normal structure responsible for sharp central and peripheral vision.
Routine eye examinations are crucial for people with diabetes, even when vision seems stable. Detecting subtle changes early allows for timely intervention and reduces the risk of severe vision loss.
Partial or Sudden Vision Loss
In advanced stages, significant bleeding or retinal detachment can lead to partial or sudden vision loss. You might experience a dark curtain-like shadow over part of your vision or a sudden drop in clarity. This is considered a medical emergency and requires immediate attention.
Sudden changes often indicate proliferative diabetic retinopathy, where abnormal new blood vessels form and increase the risk of complications.
Blurred or Fluctuating Vision
One of the most common early symptoms is blurred vision.
You may notice that your eyesight becomes unclear when reading, using a computer, or focusing on distant objects. This blurriness can come and go, especially when blood sugar levels fluctuate.
Fluid leakage into the retina may cause swelling in the macula-the area responsible for detailed central vision. This swelling can distort images and make fine tasks more challenging. If your glasses prescription seems to change frequently without clear explanation, it may be worth discussing with an eye specialist.
Dark Spots or Floaters
Small specks, cobweb-like shapes, or dark spots drifting across your field of vision can be another warning sign.
These floaters may occur when tiny blood vessels bleed into the vitreous, the gel-like substance inside the eye. While occasional floaters can be normal, a sudden increase in their number should not be ignored.
A noticeable cluster of floaters, especially when accompanied by blurred vision, may indicate more advanced changes.
Impaired Night Vision
Difficulty seeing clearly in dim lighting is another potential symptom. You might struggle more than usual when driving at night or moving through poorly lit rooms. Reduced night vision can occur when retinal blood flow is compromised. As the condition progresses, sensitivity to glare may also increase, making headlights or bright lights uncomfortable.
Distorted or Wavy Vision
Straight lines appearing bent or wavy can signal swelling in the macula. This distortion may make reading text or recognizing faces more difficult. Objects may look slightly misshapen or unclear in the center of your vision.
Macular involvement is a serious concern because it affects the most detailed part of sight. Prompt evaluation is necessary if you notice these changes.
Risk Factors That Increase Symptoms
Certain factors increase the likelihood of developing retinal complications. Poorly controlled blood sugar levels, high blood pressure, high cholesterol, and long duration of diabetes all contribute to vascular damage.
Pregnancy and smoking may also raise the risk. Managing these factors can slow progression and reduce the severity of symptoms. Maintaining consistent blood sugar control remains one of the most effective protective measures.
When to Seek Immediate Care
Any sudden change in vision should prompt urgent evaluation. Rapid onset of floaters, flashes of light, shadowed areas, or severe blurriness are signs that require immediate medical attention. Delaying care can result in permanent damage, especially if bleeding or retinal detachment is involved.
Protecting Your Vision
Preventing vision loss involves a proactive approach. Regular comprehensive eye exams, healthy lifestyle choices, and proper diabetes management play vital roles in protecting eyesight.
Modern treatments-including laser therapy, anti-VEGF injections, and surgical options-are effective when initiated early. The key is recognizing symptoms and seeking care before irreversible damage occurs.
Conclusion
Vision changes in people with diabetes should never be dismissed. Blurred vision, floaters, distortion, and difficulty seeing at night may all signal underlying retinal damage. Because early stages can be symptom-free, routine screening remains essential.
By staying alert to warning signs and maintaining good blood sugar control, individuals can significantly reduce the risk of severe vision loss. Early recognition and timely treatment offer the best chance to preserve clear, functional vision for years to come.