Arterial disease is a condition in which fatty deposits – known as plaque – build-up on the inner walls of arteries. This condition leaves narrowed, hardened arterial walls that can be difficult for blood to flow through. Peripheral arterial disease (PAD) refers to peripheral artery diseases affecting smaller vessels outside the heart or brain, such as those leading to the arms, legs, and pelvis. PAD is a serious concern because peripheral arteries carry oxygen-rich blood from the heart through the body’s network of arteries and veins to organs and tissues like muscle, skin, and bone. As such, you need to treat it seriously and visit a Davenport peripheral arterial disease specialist as soon as you develop any symptoms.
Causes
PAD is caused by the accumulation of plaque that narrows arteries over time. The causes are usually multifactorial, involving a complex interplay between heredity, lifestyle, and environmental factors such as smoking and high blood pressure. Some people develop PAD in their 30’s and 40’s without having any recognized risk factors for atherosclerosis, such as diabetes or high blood pressure.
Symptoms and Detection
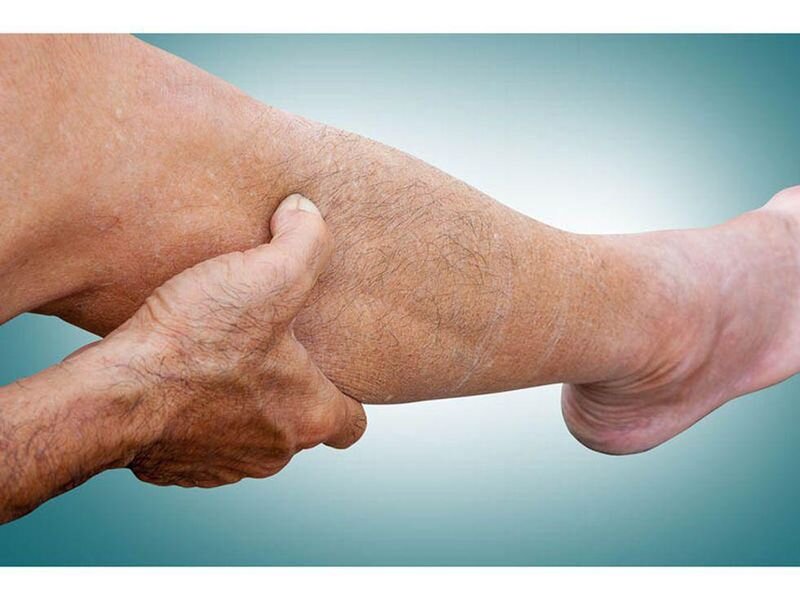
While PAD can be symptom-free, patients may experience pain or cramping in the leg muscles during walking (claudication). Claudication is brought on by physical activity and is usually relieved by rest. But if left untreated, artery disease will progress, and symptoms may become more noticeable. If you are suffering from peripheral arterial disease, you may develop symptoms such as :
- leg cramping or pain when walking
- restlessness and tiredness in the calf muscles during exercise because of restricted blood flow
- skin that itches feels numb or looks pale or blue due to a lack of circulation
- ulcers that develop on the feet and legs if not treated properly
The best way to detect PAD is through a simple medical examination. Your doctor will perform a physical exam to look for PAD signs, check your pulse and blood pressure, and order more specialized tests such as an ankle-brachial index (ABI), which compares the blood pressure in your arms to that in your legs. A low ABI value indicates arterial disease.
Treatment
The treatment of PAD is dependent on how severe your symptoms are, your overall health, and your risk factors for atherosclerosis. For example, if you have diabetes or high cholesterol, it’s essential to keep these conditions under control to prevent further narrowing of the arteries. If you smoke, talk to your doctor about ways to quit.
In some cases, PAD can be treated with angioplasty and stenting in which narrowed or blocked arteries in the legs are widened by a balloon-tipped catheter inserted into an artery under local anesthesia. This procedure usually takes about two hours, and patients can go home after one to three days.
In summary, PAD is the narrowing of arteries, making it difficult to flow. If not treated properly, the symptoms can be leg pain while walking (claudication) and ulcers on the feet and legs. If you have PAD, you may treat the condition through angioplasty and stenting, a procedure used to widen narrowed or blocked arteries in the legs. Lifestyle changes can also help.